Second Year, PL-2
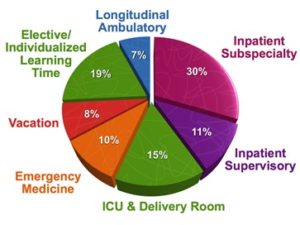
The junior year is when residents get their most concentrated exposure to subspecialty and acute care pediatrics, accompanied by an increase in decision-making autonomy and responsibility for high-acuity often critically ill patients. The junior year also introduces supervisory roles and affords more opportunities for leadership and teaching.
Increased acuity, increased autonomy: Juniors are the only residents on the following BCH subspecialty inpatient services: GI, Cardiology, Complex Care and Oncology. Breadth of subspecialty experiences is maintained by building in protected ambulatory experiences into each of these primarily inpatient subspecialty units.
Juniors also work with increased autonomy caring for acutely ill patients in the EDs at BMC and BCH, serve as the main responders to all deliveries requiring a pediatrician at BWH, and cover one of the three main teams in the Medical-Surgical Intensive Care Unit (MSICU). These rotations require juniors to build on the clinical skills and knowledge gained during the intern year, become more nuanced in their evaluations and differential diagnoses, and more independent and efficient in patient management.
Supervisory experiences: Juniors supervise interns in the BMC Ward and NICU, in the BCH Intermediate Care Program, on subspecialty teams (6 Subs: Hematology, Toxicology and End-Stage Renal Disease team; 7 Subs: Endocrine and Adolescent team; and 9 Subs: Rheumatology, Allergy/Immunology, Pulmonary and Renal teams), and on the General Pediatrics Teams (which also contains one week on the Admit team). They are also frequently role models and sources of support for interns in the ED’s at BCH and BMC. Many of our residents love to teach and lead, and these experiences are highly valued by juniors as opportunities to participate in shaping the culture of the BCRP.
Resident as Teacher Curriculum: Juniors have a two week TEACH rotation focused on developing residents’ supervisory and teaching skills. It includes scheduled activities such as delivering a chalk talk, practicing feedback, and precepting medical students, as well as provides individualized time tailored to each resident’s career goals.
Individualized Curriculum: The junior year includes 6-10 weeks elective time, of which 2 weeks are call-free. Juniors use this time to personalize their training experience by pursuing further exposure to pediatric subspecialties, dedicating time to research or teaching, engaging in global health experiences, and a myriad of other options. Some are structured by the residency program and others are individual and unique.
Expanded LEAD opportunities: LEAD residents have a half-day every month when they can choose between a second continuity clinic and a project in urban health, advocacy, global health or public policy.
PL-2 Rotation Schedule
| Service | Weeks | Night/Weekend Call |
| Supervisory Experience (BCH Gen Peds, BMC Ward, ICP, 6Subs, 7Subs, 9Subs) |
2-3 | BCH Gen Peds/BMC Ward: 3 weekend days per 3 weeks (work one full weekend + one additional weekend day, one golden weekend off) Admit: 1 week rotation, no weekend call ICP: Night float (5 nights on, 2 nights (Fri/Sat) off x 2 weeks) Subspecialty teams: 2 weeks of days (1 weekend on/1 weekend off OR 2 gray weekends (1 day off, 1 day on) |
| Inpatient Wards (GI, CCS, Cardiology, Oncology) |
2-4 (CCS) 4 (GI, Cards, Onc) |
CCS: 2 weeks of days with 1 weekend on, 1 weekend off and/or 2 weeks of nights with both weekends off (Fri/Sat nights) GI, Cardiology, Oncology: 3 weeks inpatient (one night float week), 1 week outpatient |
| Medical-Surgical Intensive Care Unit (BCH MSICU) |
2 | 2 weeks of day shifts, 1 week night shifts, 1 week outpatient. (Work 1 full weekend on days and 1 weekend of nights). |
| BWH Delivery Room (Birth and Transition Unit) |
2 | Mix of several stretches of day/night float |
| Emergency Medicine | 2-4 | Overnight shifts in 2 week blocks (5 nights on, 2 nights off) |
| TEACH | 2 | 2 weeks call-free |
| Admit | 1 | No weekend call |
| Primary Care | 2 | No night/weekend call |
| Elective | 6-10 | 2 weeks call-free, rest with weekend call (could be days or nights) |
| Sick Call/Back Up aka “Flex” | 2-4 | — |
| Vacations | Two 2-week breaks | — |
| Continuity Clinic | 1 afternoon/week on average | Increased frequency of clinic during outpatient “Y” weeks |